Parkinson’s Disease is a progressive disease, meaning the symptoms develop slowly over the course of several years. Although there are four main motor symptoms that occur with Parkinson’s, not every patient will experience symptoms in the same order and in the same way. However, there are patterns of symptom progression that most patients will experience.
The most commonly used scale to assess the stage of Parkinson’s disease is the Hoehn and Yahr scale. Named for its authors, Margaret Hoehn and Melvin Yahr, the scale was originally published in 1967 in the journal Neurology and described the progression of Parkinsonism, collection of signs and symptoms found in Parkinson’s disease, in five stages. The scale has since been modified to include stage 1.5 and stage 2.5 to account for the intermediate course of Parkinson’s.
The Hoehn and Yahr scale originally classified the five stages in the following manner:
- Stage I. Unilateral involvement only, usually with minimal or no functional impairment.
- Stage II. Bilateral or midline involvement, without impairment of balance.
- Stage III. Mild to moderate bilateral impairment with some postural instability.
- Stage IV. Fully developed, severely disabling disease; the patient is still able to walk and stand unassisted but is markedly incapacitated.
- Stage V. Confinement to bed or wheelchair unless aided.
Stages I.5 and 2.5 were later added and described as:
- Stage 1.5. Unilateral and axial involvement.
- Stage 2.5 Mild bilateral disease with recovery on pull test.
As Parkinson’s disease progresses, the symptoms start to move from affecting only one side of the body to both sides of the body before eventually causing total impairment.
Stage 1
Stage one is the mildest stage of Parkinson’s disease. Also known as early-stage Parkinson’s, in stage one, you may only have slight tremors or shaking, slowed movement, stiff limbs, and balance difficulties. Symptoms usually occur on one side of the body and don’t interfere with daily activities. There may be some changes in posture, walking, and facial expressions, that may be noticeable to friends and family members. However, often symptoms are so mild that you don’t think to seek medical attention. Or if you do seek medical attention, the doctor might not be able to make a Parkinson’s diagnosis yet.
Treatments at this stage can include physical therapy to improve balance and address muscle stiffness. Exercise is beneficial at this stage as it can help improve balance, flexibility, and strength. Dietary changes, like increasing omega-3 fatty acids and magnesium, can help reduce some of the early symptoms of Parkinson’s disease. A doctor may even prescribe medication at this stage if the benefits outweigh the risks.
Stage 1.5
In stage 1.5, Parkinson’s still only affects one side of the body, but there may be some symmetric problems on both sides, such as stooped posture, reduced arm swing, or reduced facial expressions.
Stage 2
Stage 2 Parkinson’s disease can develop months or years after stage 1. In stage two of Parkinson’s disease, the symptoms start to get worse and become more noticeable. Although balance isn’t impaired at this stage, you might experience difficulty walking and your posture might start to change. At this stage, symptoms start to affect both sides of the body. Usually, you can still live alone although some tasks might take longer to complete as movement slows down.
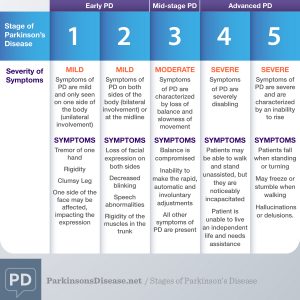

Other symptoms of stage 2 Parkinson’s disease include the loss of facial expression on both sides of the face, decreased blinking, speech abnormalities such as soft, slurred, or monotone speech, and stiffness or rigidity of trunk muscles that can cause neck and back pain. If there is no tremor present at this stage, and depending on age, it is possible for Parkinson’s to be misdiagnosed or misinterpreted as simply advancing age.
Certain medications may be prescribed during this stage to help with balance and movement issues. These include carbidopa-levodopa, which the body converts into dopamine to make up for the low dopamine levels that occur in Parkinson’s, and dopamine agonists that mimic the effects of dopamine. Another medication that might be prescribed at this stage is an MAO-B inhibitor to stop the breakdown of dopamine in the brain.
Alternative therapies such as yoga, meditation, and diet, can be beneficial during this stage.
Stage 2.5
In stage 2.5, both sides of the body are affected and there is mild impairment of balance. To test for stage 2.5, your doctor will tell you that you will be pulled backward and then you will have to take a step back to try to prevent a fall. It is expected that you’ll take one or two steps backward to prevent yourself from falling, but if you take three or more before balance is recovered, then the disease is considered stage 2.5.
Stage 3
Stage 3 is considered mid-stage and signifies a major turning point in the progression of Parkinson’s disease. Stage 3 is categorized by a loss of balance and coordination. At this stage, routine activities become more difficult to complete, such as eating, getting dressed, or bathing. Movement becomes slower and you may be unable to make the rapid, automatic, and necessary moves to prevent falling, which is why falls become more common in this stage.
Stage 1 and 2 treatments are still beneficial in stage 3, such as eating a balanced diet, exercise, physical and occupational therapy, alternative treatments, and medications. However, the effects of certain medications may begin to lessen at this stage.
Stage 4
The symptoms of Parkinson’s disease become much more severe in stage 4. While it may be possible to stand unassisted, movement is limited and may require a walker. At this stage, help is needed with daily activities and you may be unable to live alone because of decreases in movement and reaction time.
Treatments may become less effective in stage 4 and stage 5. Your doctor may decide to change the delivery of certain medications. For example, instead of taking carbidopa-levodopa as an oral dose, you might get an infusion instead. At this stage, you could potentially benefit from surgical procedures to reduce symptoms such as deep brain stimulation, which involves implanting electrodes into the brain to emit electrical pulses.
Stage 5
Also called end-stage Parkinson’s, stage 5 is the most advanced and debilitating stage. Because of advanced stiffness in the legs, walking and standing is almost impossible. Patients have severe posture issues in the back, hips, and neck, and might be bedridden. You may require a wheelchair and may not be able to stand on your own without falling. Around-the-clock nursing care is needed for all activities.
How are the different stages of Parkinson’s treated?
Treatment for Parkinson’s depends on the severity of the symptoms. In the early stages, prescription medication may be enough to treat more mild symptoms. A 2019 review published in the journal Biomolecules listed some of the main pharmacological treatments for motor and non-motor symptoms for each stage of Parkinson’s disease.
The main pharmacological treatments include medications such as l-dopa, a precursor to dopamine that crosses the blood-brain barrier to increase dopamine transmission, clonazepam or melatonin for REM sleep behavior disorder, and SSRIs (selective serotonin reuptake inhibitors) or SNRIs (serotonin and norepinephrine reuptake inhibitors) for depression, which is a common non-motor symptom for Parkinson’s. About 50% of people with Parkinson’s experience depression.
L-dopa is the most effective and most prescribed medication for Parkinson’s. Although it doesn’t slow the progression of the disease or cure it, it can help control movement symptoms such as slow movement (bradykinesia), rigidity, and tremors. However, one of the side effects of l-dopa is dyskinesia, strange, jerky movements that can’t be controlled. You might decide to hold off on starting l-dopa if your symptoms are not getting in the way of your daily life.
Another common treatment for early and advanced Parkinson’s disease is amantadine. Initially developed as an antiviral medication to treat influenza, clinical trials confirmed that it could also be used to treat Parkinson’s symptoms. It can cause greater amounts of dopamine to be released in the brain. Amantadine can help improve rigidity and slow movements, as well as dyskinesia, and may be combined with other medications in later stages.
Additional treatments for Parkinson’s may include medications like dopamine agonists and monoamine oxidase inhibitors, and non-pharmacological treatment like physical therapy and speech therapy.
Are there limitations to the Hoehn and Yahr scale?
One of the main limitations of the Hoehn and Yahr scale is that it focuses solely on motor symptoms. While Parkinson’s primarily affects movement functions, it can have other symptoms such as sleep changes and restless leg syndrome, or cognitive changes such as mood changes, fatigue, loss of smell, and micrographia (small handwriting). Some patients with Parkinson’s disease may also experience hallucinations or delusions.
To account for non-motor symptoms of Parkinson’s disease, there is another rating scale known as the Unified Parkinson’s Disease Rating Scale (UPDRS). Neurologists developed the UPDRS in 1987 as a gold standard for monitoring the response to medications used to decrease the signs and symptoms of Parkinson’s disease. The scale contains four parts:
- Part I: Mentation, Behavior, Mood
The first part scores intellectual impairment, thought disorder, depression, and motivation/initiative.
- Part II: Activities of Daily Living
The second part scores activities such as hygiene, dressing, walking, tremor, and sensory complaints.
- Part III: Motor Examination
The third part scores speech, facial expression, tremor at rest, hand movements, and other motor functions.
- Part IV: Complications of Therapy (in the past week)
The final part scores whether and how often the patient experiences symptoms such as painful dyskinesias, dystonia (involuntary muscle contractions), nausea, vomiting, or sleep disturbances.
Parts I to III of the UPDRS are scored on a 0-4 rating scale, and Part IV is scored with yes or no ratings. The higher the score, the more severe the symptoms. The highest possible score, 199, represents total disability, while a score of 0 represents no disability.
After the UPDRS is completed, an administrator will complete the Hoehn and Yahr Standing Scale and the Schwab and England Activities of Daily Living Scale. The latter is scored by percentages, with 100% being completely independent and 0% being bedridden with vegetative functions now functioning.
Getting Care at Any Stage
Although the different scales are meant to measure the progression of Parkinson’s disease and the response to medication and treatment, some patients may never progress to stage 5, and not everyone with Parkinson’s will spend the same amount of time in each stage. Some people are diagnosed with Parkinson’s when they are young and remain in the early stages for several years. Others may skip stages, or their progression to end-stage Parkinson’s may be more rapid. It is also possible to experience symptoms like tremors but not have any balance issues.
No matter where you are in your Parkinson’s journey—whether you’re at stage 1 or stage 5—know that you’re alone. At PLM, there is a community of over 30,000 Parkinson’s patients who know what you’re going through. Join the conversation to connect with others who are like you and can support you through your illness.
