Ever wonder how many patients like you are using drugs off-label? Or how hard is it to take MS medications as prescribed? You’re about to find out.
In January, the PatientsLikeMe R&D team published not one but two studies in the Journal of Medical Internet Research (JMIR) in an effort to provide answers about how patients like you are actually using your treatments. We’ll highlight both studies here on the blog today and tomorrow. (Note: Because JMIR is an open-access journal, the articles are free for you or anyone to read in full, without fees or subscriptions or a library card.)
Study One: Off-Label Drug Usage
Our first study looked at the rates of off-label drug usage in our communities. What do I mean by “off-label”? When a drug is approved by the FDA (or outside of the US, by other regulators such as the EMEA), it is “indicated” for the treatment of a specific condition, which permits the manufacturer to market it to doctors who treat that condition and patients diagnosed with it. This indication is described on the medication’s label.
Any physician may choose to prescribe a treatment for a purpose that has not been indicated, however. This is known as “off-label” use. Manufacturers are not allowed to promote such use, though, and because most research focuses on new drug development, there are few systematic ways to discover how common off-label drug use is or to quantify its effects. Yet at PatientsLikeMe, thousands of patients like you are sharing data on this very practice. So, the R&D team decided to take a closer look.
This led to our JMIR study entitled “Patient-reported Outcomes as a Source of Evidence in Off-Label Prescribing: Analysis of Data From PatientsLikeMe” (which I am proud to report was the winner of the inaugural Medicine 2.0 award). We started by identifying two widely used drugs to study: amitriptyline (a tricyclic antidepressant indicated for the treatment of depression) and (a wakefulness-promoting drug indicated for the treatment of narcolepsy). Then, we examined how patients like you were using them used across five condition-based PatientsLikeMe communities: MS, fibromyalgia/chronic fatigue syndrome, ALS, mood disorders (depression, bipolar disorder, and anxiety disorders) and Parkinson’s disease.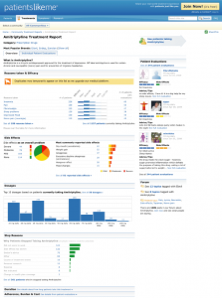
Our data revealed that less than 1% of almost 2,000 patients taking modafinil and only 9% of nearly 1,400 taking amitriptyline are taking each drug for its approved indication. That means the vast majority of you are taking these drugs “off-label.” You also reported higher perceived efficacy for off-label uses than for approved indications, surprisingly. Another interesting discovery is that many of you cited what are normally considered the side effects of amitriptyline (e.g. dry mouth) as your purpose for taking the drug (e.g. to treat excessive saliva).
If researchers are only looking at clinical trial data, they’re missing the whole story because they don’t know what’s being prescribed off-label. To be clear, off-label prescribing is commonplace and standard practice in many conditions, with safety and efficacy established by clinicians’ experience rather than formal studies. However, whenever we can improve upon the status quo by unlocking a new data source (such as what you share via our site), we should seek to maximize that information.
Up next tomorrow…how you’ve helped develop patient-reported outcome instruments.

Pingback: Tweets that mention The Value of Openness: The PatientsLikeMe Blog » How Patients Like You Use Your Treatments in the Real World: Two New Studies -- Topsy.com
Pingback: The Value of Openness: The PatientsLikeMe Blog » How Patients Like You Use Your Treatments in the Real World (Cont’d)
Pingback: The Patient Graph | Jay Caplan on Medical Devices
Pingback: Components of a Personal Vitality Score | Health Information Economy | Goel Insights